Modern ceramic dental implants, when correctly positioned and handled, represent a highly innovative addition to the treatment spectrum in dental implantology.
In the past, ceramic dental implants were usually regarded as part of a more holistic approach to dentistry due to the stigma of them being ‘metal-free’. Today however, they also provide an additional option in the treatment spectrum of the general implantology practice and they are one of the biggest innovations in dentistry. Thus, the number of contributions about ceramic implants in specialised publications and scientific conferences has been growing. The reason for this development has already been mentioned several times throughout expert literature – the increase in patient demand for metal-free restorations plays a role as well as the fact that zirconia as a material brings tangible professional benefits.
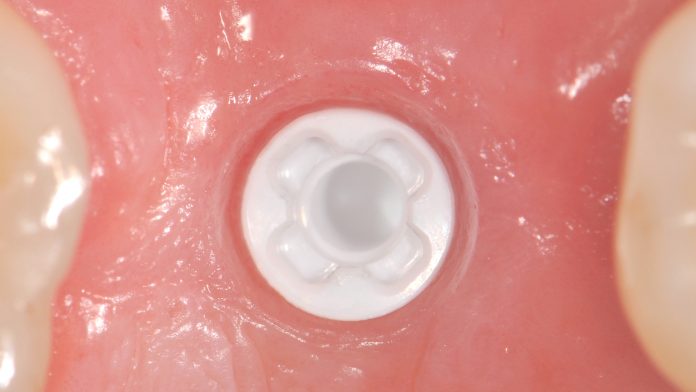
For the replacement of missing teeth, ceramic dental implants represent an innovative and modern treatment option in dentistry. An implant is usually a screw that is inserted into the jawbone with a minor surgical procedure and serves as a replacement for the tooth root. After three months of healing time, the implant is firmly attached to the bone (known as ‘osseointegrated’). At this point, a new crown or denture is attached to this artificial tooth root. With a two-part implant, the current standard for titanium implants, an abutment is first attached to the implant with a small internal screw. A one-piece implant is considered to be a single-piece implant, if the implant and abutment are firmly connected from the beginning and the entire system has been manufactured from one part.
The first titanium dental implants were inserted as early as 1965. With today`s success rates of 98.5% after 10 years, they still represent a successful and save concept in medicine. In contrast to other materials, titanium is particularly biocompatible and forms a direct connection with the bone (osseointegration), which under normal, infection-free conditions ensures this high reliability. The first ceramic implants were introduced almost at the same time by Professor Sami Sandhaus in 1967. However, the material aluminium oxide used until 2000 led to high fracture rates and, in the early days, smooth implant surfaces and thus low osseointegration led to high loss rates which are no longer acceptable today. This situation began to change with the introduction of zirconium dioxide as a reliable implant material and modern surface treatment.
However, ceramic dental implants are increasingly losing their reputation as a niche product and are finding their way into general implantology practice. This is not least due to increased health awareness among the population and the resulting rise in demand for metal-free restorations. A major reason for this development is also the increased acceptance by dentists working in implantology. The technological innovations in materials, surface design and treatment protocols now make it possible to implement the clinical advantages of zirconium dioxide in daily practice for the benefit of patients. Considering the evidence-based indications ‘single-tooth restoration’ and ‘three-unit bridge’, survival rates for most modern ceramic systems are already on a par with titanium implants. However, long-term data must confirm the promising short and medium-term results.
Why ceramic dental implants?
One of the most frequently cited advantages of ceramic implants relates to aesthetics. With a ‘grey’ titanium implant, a thin covering of soft tissue can cause the metal to shimmer through in a grey, dark colour. This can be avoided with the white ceramic material, which has great advantages, especially in the visible anterior region. Of course, excellent aesthetics can also be achieved with titanium implants. However, the prerequisite for this is the presence of at least 2mm thick gums, which prevents such a greyish shimmering through of the titanium implants. If this is not the case, the soft tissue must be thickened with connective tissue grafts, which means an additional intervention and thus an additional burden for the patient.
Even if further scientific evidence for this must be provided, the main argument in favour of ceramic implants, at least from clinical experience, is the excellent and almost completely inflammation-free soft tissue situation around the implant.
According to initial findings, the reasons for this at least subjectively improved peri-implant soft tissue situation are the good biological properties of the ceramic:
- Compared to titanium, the ceramic material shows less plaque and bacterial accumulation;
- The circular blood circulation of the soft tissue around the implant also corresponds more to the natural tooth with ceramic and is significantly reduced with titanium; and
- It is well known that better blood circulation means healthier soft tissue and healthier soft tissue in turn not only results in improved aesthetics.
Even if the corresponding long-term evidence for ceramic implants is still lacking, the first three and five year results are already available, and the trend is supported by clinical observation. Gingivitis (periimplantitis) around the implant, which is observed with titanium implants with a high prevalence of up to 14.5% over 10 years and which can lead to implant loss, could not yet be clinically described with ceramic implants. One reason for this seems to be the lack of corrosion of zirconium dioxide, as described for titanium dioxide as biocorrosion. Titanium dioxide particles released by corrosion and abrasion are phagocytised by monocytes of the immune system. The result is an increased release of inflammation mediators and thus increased inflammation and bone resorption. This fact ‘less periimplantitis’ is the main argument in favour of ceramic implants.
The material zirconium dioxide
As good as these arguments may be for ceramic implants, the long-term stability of the implants must be guaranteed in order to be able to make use of these advantages. This stability depends largely on the material properties and the healing behaviour of the implants.
In this area, particularly in the areas of implant material, design of the implant surfaces and the treatment concepts, a rapid further development with many innovations has taken place, whereby today the success rates depending on the implant system and study design are up to 98% in the area of titanium implants. Even the fracture rates, which used to be quite high, have been revised by the introduction of innovative materials in both static and dynamic fracture strength tests according to ISO 14801.
It should be noted that zirconium, like titanium, is also a metal. Oxidation with oxygen produces the ceramic ‘zirconium dioxide’. This process is not reversible – no metallic zirconium can be formed. However, not all zirconium dioxide is the same. There are still major differences in the manufacturing process, material selection, surface design, restorative concepts and handling of individual systems.
Modern ceramic implants consist of TZP ceramic (tetragonal zirconium dioxide polycrystals) with an average bending strength of 1,100 MPa. In order to increase the bending strength to 1,200 MPa and to positively influence the ageing process (hydrothermal degradation), up to 0.5% by volume aluminium oxide was added (TZP-A). If the volume percentage of aluminium oxide is increased to 20%, new hybrid ceramics are created which achieve a flexural strength of up to 2,000 MPa. This ATZ-ceramic (Alumina toughened Zirconia) significantly reduces the risk of fracture in addition to the already highly resistant TZP-A. The aging process due to hydrothermal degradation has hardly any clinical relevance anymore due to these procedures.
Whether TZP, TZP-A or ATZ, the further processing of the starting material is important. Grain size, purity and density have a decisive influence on hardness and quality. Two basic methods can be distinguished in the manufacturing process. In the first process (CIM – Ceramic Injection Mold, CIP – Cold Isostatic Pressing), first of all the shaping is carried out by injection molding or green body processing and in the second step the refinement by the sintering process.
In the other process (hard-machining), the process is reversed – first, a block is compressed and thus refined in the HIP process (Hot Isostatic Post Compaction) under high pressure of up to 2,000 bar and temperatures of up to 2,000°C. Only then is the mould ground from the finished blank at high industrial cost. Very high-quality and precise results can be achieved in both processes.
Surface design and renaissance of the ceramic implants
The bone-implant contact (BIC) plays an important role in reliable healing. The larger an implant surface is, the more bone cells can attach themselves to it, and the stronger the bond between implant and bone. Since the volume of the implant itself cannot be increased, the surface of the implants is now increased by ‘roughening’. Whereas in the early stages of ceramic implants only smooth, machined surfaces were used, today modern processing methods, modified in various ways, ensure rougher implant surfaces, which are up to ten times larger. High-grade corundum radiation, thermal acid etching, laser modulation or preliminary structuring by the press mould stand for a BIC, is almost equivalent to titanium implants and thus show equivalent osseointegration.
The developments and innovations in ceramic implantology described here, and their increasing relevance, have also been recognised by the industry. Almost all renowned implant suppliers have currently included ceramic implants in their product portfolios, which has led to ever higher quality products and to a ‘renaissance’ of ceramic implants as a result of a high level of research. The advantages of this development for the patient are obvious – less inflammation and better aesthetics with long-term stability. However, these systems must also be practically applicable for dentists and their handling should be as similar as possible to that of titanium implants. However, there are still differences in the various systems due to the material.
One-piece ceramic implants
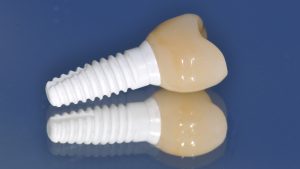
One-piece ceramic implants currently still have a higher evidence base than two-piece systems, as most studies refer to one-piece systems due to their longer availability. In one-piece systems, abutment and implant consist of one piece (monobloc), which means they are considered hermetically sealed (no abutment necessary, no separate abutment connection, and no implant interface). They have the advantage that they come very close to the crown restoration of a natural tooth in the restoration of the usual work of the dentist with impression and cementation
The restorative treatment on one-piece implants is carried out exclusively by cementing the restoration. Cement removal deeper than 1.0mm to 1.5mm below the gingival margin is no longer reliably guaranteed. One-piece implants must be positioned accordingly, otherwise remaining cement residues may lead to inflammation (also referred to as ‘cementitis’).
Two-piece ceramic implants
As already described, two-part systems are state of the art in general titanium implantology. They cover almost all indications, enable unloaded healing phases, primary wound closure, single-stage augmentation procedures and are both reversible and flexible.
With titanium implants, the connection of implant and abutment is relatively easy to achieve by means of elastic ‘metal-to-metal’ connections. However, this connection of hard, non-elastic zirconium abutment with hard, non-elastic zirconium implant still represents one of the greatest challenges for the two-part design of ceramic implants.
Two-piece ceramic implants are screwed together by means of the metal screws made of either gold or titanium, which have also been commonly used for titanium implants. Since wear and abrasion of the screw can occur in the hard internal implant thread due to micro-movement of the screw (which is softer than the ceramic screw), the precision of the implant-abutment connection and the screw fit is decisive for success.
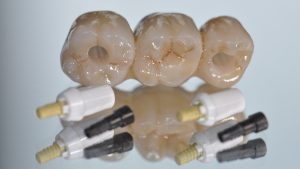
Two-piece metal-free screw-retained ceramic implants
A new approach and a particularly innovative concept is being pursued in this respect with the screw connection using carbon fibre reinforced abutment screws. In these screws, carbon fibres with a volume fraction of more than 60% are embedded in a PEEK matrix, which enables a particularly high tightening torque of up to 85Ncm. The threads of the screw are rounded on the flanks and distribute the forces that occur evenly in the implant body.
Thanks to this two-part concept, the workflows familiar from titanium implants can now be retained in both the dental practice and the dental laboratory for handling ceramic implants – unloaded and covered healing, open or closed impression, precise model fabrication, individualization of the abutments, metal-free and reversible screw connection for a wide range of indications.
Conclusion
Compared to titanium implants, ceramic implants have a lower existing evidence level. Further studies must follow to confirm the promising short and medium-term results. Nevertheless, within the framework of the data already available today, it can be stated that in addition to the success prognoses, ceramic implants have also come closer to titanium implants in terms of handling. The knowledge gained from titanium implantology and the biological principles also apply to ceramic implants. Bone augmentation, for example, can also be used with the same procedures.
Any familiar surgical and prosthetic protocols can be adopted as far as possible – besides evidence and reliability, this is certainly an important argument for the future acceptance of ceramic implants in dental implantology. Thus it can already be stated today that modern ceramic implants, when correctly positioned and handled, represent a highly innovative addition to the treatment spectrum in dental implantology and will continue to gain in importance for the benefit of patients in the future. This has to be supported by a scientific and evidence-based approach, as the European Society for Ceramic Implantology (ESCI) has set itself the goal.
Dr Jens Tartsch
President
European Society for Ceramic Implantology (ESCI)
dr.tartsch@zahnarzt-kilchberg.ch
www.esci-online.com/en/
www.zahnarzt-kilchberg.ch
Please note, this article will also appear in the second edition of our new quarterly publication.