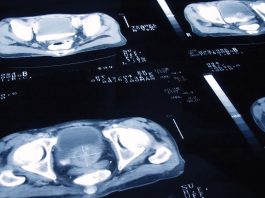
Becky Campbell and Jason Musni from the Prostate Cancer Foundation discuss prostate cancer – from the basics to cutting-edge research.
Cancer is a condition in which a normal cell starts to grow uncontrollably without having the signals or ‘brakes’ that stop cell growth. Prostate cancer starts in the prostate, a small gland located below the bladder that is responsible for secreting one of the components of semen.
In many cases, prostate cancer is relatively slow-growing, which means that it often takes years to become large enough to be detectable and even longer to spread outside the prostate, or metastasize. However, some cases are more aggressive and need more urgent treatment.
In the United States, the majority of prostate cancers are discovered at a local or regional stage, and the five-year relative survival rate is 99%. The five-year survival for disease diagnosed at a distant stage is 30%. In England, nearly nine in ten of men diagnosed with prostate cancer survive for five years or more; survival has improved greatly over the last four decades. Incidence and mortality vary across the EU, with generally higher rates of diagnosis in Northern and Western Europe.
Diagnosis and Risk factors for prostate cancer
The PSA blood test and digital rectal exam (DRE) can be used to detect prostate cancer when no symptoms are present. They can help catch the disease at an early stage when treatment may be more effective and potentially has fewer side effects. Use of these screening measures may differ by country and regional health system.
Risk factors for prostate cancer include:
- Increasing age;
- African ancestry;
- A family history of the disease; and
- Certain inherited genes.
Having a family discussion about cancers on both maternal and paternal side may help shed light on the types of cancer screenings family members need. Lifestyle matters, too: there is evidence that smoking increases the risk of fatal prostate cancer and excess body weight increases the risk of aggressive and fatal prostate cancer.
Treatment: no one size fits all
There is no ‘one size fits all’ approach for the treatment of prostate cancer. It is important for a man to learn as much as possible about the treatment options available and, with his doctors, make a shared decision about what is best for him. Treatment options depend on how aggressive the disease appears on a biopsy (from ‘very low’ to ‘very high’ risk), whether the cancer has spread outside the prostate at the time of diagnosis, and patient factors and preferences.
A man diagnosed with localised or locally advanced prostate cancer (cancer that is in the prostate or the region around it) has three primary treatment options:
- Active surveillance;
- Surgery; and
- Radiation therapy.
Active surveillance is a strategy to follow the cancer closely with regularly scheduled PSA checks, DREs, and biopsies so that treatment is deferred to only ‘if and when’ it may be needed. Surgery entails removing the entire prostate gland and seminal vesicles, known as a radical prostatectomy. This is an option for men with intermediate or high-risk cancer that has not spread. Radiation therapy precisely kills cancer cells with ionising radiation. Like surgery, it is very effective for localised or locally advanced prostate cancer and has the same cure rate as surgery.
For men whose disease appears more aggressive, certain treatment combinations may be recommended. Hormone therapy may be added. Also known as androgen deprivation therapy (ADT), this is medication to stop testosterone from being produced or to directly block it from acting on prostate cancer cells.
Along with their doctors, men must carefully evaluate the risks, benefits, quality of life concerns, and all other factors before making this choice. For example, while one man might be more concerned about returning to work quickly, another man might focus on maintaining long-term erectile function or urinary continence.
In some cases, prostate cancer is more aggressive and has spread outside the prostate (metastatic) at the time of diagnosis. It can also recur months or years after initial treatment. Fortunately, men with advanced prostate cancer have several treatment options, including ADT alone or in combination with newer ‘second generation’ anti-androgen medications. For patients with a low volume of metastatic disease at diagnosis, radiation therapy may be combined with ADT. Prostate cancer chemotherapy drugs can help manage pain in patients with metastatic disease. Currently, taxane chemotherapy is a standard of care for men with metastatic prostate cancer that has spread and is progressing despite hormone therapy. Other, newer treatments include immune checkpoint inhibitors, a prostate cancer vaccine (sipuleucel-T), and bone-targeting treatments such as radium-223. Availability of these therapies may vary.
Side effects of treatment
Because the prostate is close to several vital structures, localised prostate cancer and its treatments can disrupt normal urinary, bowel, and sexual functioning. Prostatectomy may result in urinary incontinence or leakage. Nearly all men will have some form of leakage immediately after the surgery, but this will improve over time and with strengthening exercises. Radiation therapy may cause a mild increase in urinary frequency and urgency, and/or the need to urinate during the night.
After any of the most common prostate cancer treatments, fertility is unlikely. After surgery, orgasm may still occur (without ejaculation) but natural conception will not be possible. Radiation similarly destroys the prostate and seminal vesicles; chemotherapy and hormone therapy are both harmful to sperm production.
Erectile dysfunction remains the most common side effect after treatment. This is because the nerves and blood vessels that control the physical aspect of an erection are incredibly delicate. Fortunately, many excellent treatments for managing erectile function exist on the market today.
For advanced treatments, there are other side effects. ADT causes side effects related to reversing all of the normal functions of testosterone. Although most men may experience only a few of these symptoms, the list of potential effects is long, including hot flushes, decreased sexual desire, metabolic changes, and changes in mood and thinking.
For chemotherapy, reactions to drugs can vary widely, so it is important to pay attention to any side effects. The chemotherapy drug docetaxel is well-tolerated, and many men are surprised to find that disease-related symptoms (pain, fatigue, loss of energy) are improved. Perhaps the most serious side effect of docetaxel is fever, with a low white blood cell count that requires medical attention and can be life-threatening. This occurs in 5-10% of men. Certain medications may reduce this risk.
Living with prostate cancer
If you are living with prostate cancer, make sure to take care of your whole self. Here are some key tips:
- Communicate – your family and friends want to support you. Keeping open channels of communication is key. Agree on how to make decisions, get ready for changes in routine, and understand it may be an emotional time for everyone. Communicate with your treatment team, especially about side effects, which can include mood or cognitive changes, too, not just physical ones;
- Maintain wellness – from the moment you are diagnosed with prostate cancer, it is important to make mindful decisions about your diet and lifestyle. Your everyday choices are vital to the success of your treatment and your recovery from the disease;
- Eat well and exercise – there is growing scientific evidence that suggests healthy diet and lifestyle practices may actually slow the growth and progression of prostate cancer. If you smoke, quit. A whole-foods diet with a foundation of brightly-coloured vegetables and limited animal products decreases chronic bodily inflammation and may lower cancer risk. Vigorous exercise may reduce the risk of prostate cancer death. Find out about the latest in lifestyle research at pcf.org/guide; and
- Take stock of your mental health – living with prostate cancer can affect the way you view yourself and affect your interactions with the world around you. Many patients choose to attend patient support groups or begin working with a mental health practitioner. Others feel more comfortable connecting one-on-one with another prostate cancer survivor.
The future of prostate cancer treatment
Precision medicine uses new diagnostic tests to treat the right patient with the right medicine at the right time based on the unique biology of that patient’s cancer. The promise of precision medicine is this: someday, there will be no trial and error for prostate cancer drugs.
The Prostate Cancer Foundation (PCF) plays an integral role in developing cutting-edge treatments and precision technologies to prevent, detect, and treat prostate cancer. For example, PCF funded early work that led to the development of PARP inhibitors, medications that may benefit men with metastatic prostate cancer who have specific mutations in certain genes that repair DNA.
The future of prostate cancer treatment lies in clinical trials, which move new treatments to patients who need them most, and secure data, so that regulatory approval can be obtained and new drugs can enter widespread clinical practice.
Becky Campbell
Jason Musni
Prostate Cancer Foundation (PCF)
+1 310 570 4700
info@pcf.org
Tweet @PCFnews
https://www.pcf.org/
Please note, this article will also appear in the second edition of our new quarterly publication.